Based on my many discussions with breeders over the years, there appears to be a great deal of misunderstanding about the bacterial disease brucellosis. Interestingly, there also seems to be misunderstanding at some veterinary offices as well.
Brucellosis is a contagious disease caused by the bacterium Brucella canis. It is one of the leading causes of infertility in breeding stock. It occurs worldwide, affects all kinds of dogs, purebred and not, and can also be transmitted from dogs to humans. Other animals that can be affected with brucellosis include livestock such as sheep, cattle, and goats, as well as wildlife, including bison, elk, and wild pigs.
In dogs, a classic sign of brucellosis is abortion during the third trimester of pregnancy. Other signs include stillbirths, conception failures, and litter resorption. Some infected dogs may show no symptoms, however.
In humans, clinical symptoms vary. They range from mild, nonspecific or flulike symptoms to infertility or serious cardiac or neurological problems.
In dogs, the bacteria tend to attack the reproductive organs (steroid-dependent tissues) but can also migrate to the eyes, spinal column, liver, spleen, and lymph nodes.
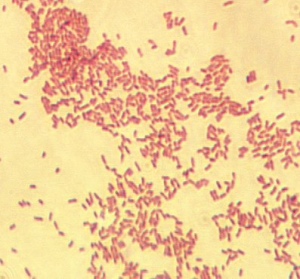
Microscopic view of Brucella (Tufts University)
About Brucellosis
With dogs, the main mode of transmission of brucellosis is by direct contact with infected body fluids, such as semen, vaginal secretions, and urine. Aborted materials are also a major source of infection. The bacterium invades the body via the mucous membranes of the genitals, nose, eyes, or mouth and is spread throughout the body (organs) via blood and lymph nodes.
Brucellosis affects female and male dogs in specific ways:
Females: The most often seen clinical symptom in the female dog is infertility, with 75 percent of cases resulting in late-term abortion (45–55 days of gestation). Aborted puppies will typically show signs of generalized infection, with the female presenting a brownish or green-grey discharge and being highly contagious with the bacteria for several weeks.
Males: The male will present with severe inflammation and/or infection of the epididymis (that part of the testicle where sperm matures and is stored). In the early phase of infection, the testes will be enlarged and painful. As the infection progresses, the testes become firm and shrunken. Infected males will become sterile due to testicular damage causing anti-sperm antibody formation.
Infected males may also develop prostatitis (inflammation of the prostate gland), with clinical symptoms of difficulty urinating and defecating.
Both sexes: Non-reproductive symptoms in both sexes can include lethargy, weight loss, and exercise intolerance. More specific clinical symptoms will depend on the organ infected but can include inflammation of the spine, eye, heart, and skin.

The Importance of Testing
There are accurate, definitive tests for brucellosis (PCR-based, blood culture), but they must be performed correctly. Screening tests are accurate if negative except very early in the course of the infection. (There is not a 100-percent accurate, definitive test for this infection in dogs, though there are many tests available.)
A simple blood draw is most often used. The rapid slide agglutination test (RSAT) that detects antibodies to Brucella spp. is often used as a screening tool. This test is quick and inexpensive, but cross-reactivity with other bacterial species commonly results in false positives. Therefore, if the test is positive, it is important to confirm the results with another test that is more specific for Brucella spp. antigens.
A definitive diagnosis can be made by positive culture of the bacteria in blood or tissue. However, the bacterium is difficult to detect in early stages with antibiotic treatment affecting the results. PCR testing can confirm the presence of active infection by detecting DNA of the Brucella spp., but lab tests are not yet universally available. Ultrasound and/or X-rays may help show abnormalities in the prostate and/or testicles, and inflammation of the spine in cases of discospondylitis.
Sadly, there is no guaranteed cure for this infection in dogs. It is very difficult for antibiotics to effectively penetrate cells to eradicate the disease. Long-term doses of combinations of antibiotics have been tried, as well as neutering and isolation of infected dogs, but the infection often reappears. As the disease is zoonotic (capable of spreading to humans), tragically, euthanasia of infected animals is recommended.
The foregoing should alert breeders as to just how imperative it is to test both male and female dogs for brucellosis before breeding.

Procedures and Prevention
When abortions, infertility, and/or testicular abnormalities are detected in dogs and/or bitches during routine inspections or testing, immediate blood testing for Brucella canis should be done. (Again, it is important to bear in mind that positive results can be false and need more specific testing.)
Your veterinarian should know how to accomplish this testing. The kennel should be quarantined during the eradication process, with no new dogs brought to the premises and no selling, relocating, or breeding. Serology testing should be done on all animals in order to identify the sources of infection.
Any animal testing positive must be immediately removed. Monthly testing must then continue for at least three months, until there are no new positive results for brucellosis.
After this period, testing should be performed every three months for a year and a preventative plan put in place. Very thorough and careful hygiene routines are vital if this disease is to be eradicated. Sadly, there is no cure, and even if tests are showing a negative result, the infection will most commonly recur.
All organic material should be removed from infected surfaces prior to a thorough disinfection. It is essential that dogs testing positive are not kept as breeding stock, even if they are of great genetic importance in a breeding program. The only way to have and to successfully maintain a clean environment for the dogs is if all infected dogs are removed.
Prevention is easily accomplished by simple blood testing of both the dog and bitch prior to breeding. Stud dogs must be tested annually, and bitches must be tested prior to each breeding. This serological test should even be done on a stud dog being collected for frozen semen. Any new animal entering the premises should be quarantined for 8–12 weeks and tested for Brucella canis at the beginning and the end of the quarantine period.
Brucella canis is not transmitted only by sexual activity; all maiden bitches and virgin dogs should also be tested. The bacteria can be found not only in the reproductive tract but also in the eyes, spinal column, liver, spleen, and lymph nodes. The main route of infection is by direct contact with infected body fluids, such as semen, vaginal secretions, and urine.
To date, there is no vaccine for prevention of the disease in dogs.
Risk to Humans
Canine brucellosis is a reportable disease in many states (though not California). In the event of a positive blood result, your veterinarian can seek advice from the state veterinarian regarding a plan of action. It is important to keep in mind that false positives occur, and in this case re-testing or testing at a different laboratory is needed. It is imperative to confirm that a positive result really is positive.
Since the disease can be transmitted to humans, and for dogs there is no known cure and no vaccine, infected dogs are a health hazard to humans. While most human cases of brucellosis are caused by consuming unpasteurized dairy products or undercooked meat, it is possible for humans to get this disease from dogs. Most reported cases from a canine source have been from people who have had direct contact with an aborted litter or aborted material associated with such a litter, such as veterinary technicians and breeders.
Immune-compromised people are at the greatest risk and are of particular concern for contracting this disease. Pregnant women and young children are also at the top of the “concern” list.
Clinical signs in people range from being uncomfortable with flulike symptoms to septicemia, infertility, and cardiac and neurological symptoms of a more serious nature. Fortunately, humans do respond to antibiotic treatment, but prolonged therapy is required. (See the CDC website for more information.)
The above is based on interviews with and articles by Autumn Davidson, DVM, MS, Diplomate ACVIM, VMTH SAC, School of Veterinary Medicine, University of California, Davis.
—Carolyn R. Gold, Gordon Setter Club of America, from a two-part article in the April and July 2015 AKC Gazette
This article is intended solely as general guidance, and does not constitute health or other professional advice. Individual situations and applicable laws vary by jurisdiction, and you are encouraged to obtain appropriate advice from qualified professionals in the applicable jurisdictions. We make no representations or warranties concerning any course of action taken by any person following or otherwise using the information offered or provided in this article, including any such information associated with and provided in connection with third-party products, and we will not be liable for any direct, indirect, consequential, special, exemplary or other damages that may result, including but not limited to economic loss, injury, illness or death.


